In all of EMERGENCY's facilities around the world, we invest in women’s professional development -…

Doctor Tony in Iraq: Health Promotion in Ashti Camp Part One
 My name is Tony Bruno, but they call me Dr Tony around here.
My name is Tony Bruno, but they call me Dr Tony around here.
I work for EMERGENCY NGO, an Italian-based, international humanitarian organisation focused on treating civilian victims of war. While I call Calgary, Canada home, I was stationed in Sulaymaniyah, Iraq for 6 months providing care for the sick and wounded, and training local doctors in 3 refugee camps. The latest numbers I’ve read is that there are over 3.3 million internally displaced people (IDPs) in Iraq, of which about 500,000 live in critical share arrangements (unsafe, unfinished buildings) and 750,000 live in some 30 refugee camps.
We currently serve around 25,000 people in 3 camps. Iraqi Kurdistan’s population of 5.2 million have opened their arms to hundreds of thousands of displaced families of different religions and ethnicities, providing housing, water and electricity services, and constructing schools, health centers, and transport offices. Can you imagine living in a place where 1 in 4 people living there is a refugee or IDP? I can because I did. The sites and stories I saw and heard daily are heart breaking. But getting to know and serve these victims and casualties of war is the reason I went to Iraq. This is my purpose and I am honored to help.
The work my colleagues and I do in Iraq is the most emotionally and spiritually demanding job I’ve ever done, but I’ve also have never been so inspired in my life. I look forward to sharing this journey with you.
… Ready
In this series of posts, I want to take you on the journey of a de-worming campaign in the camps we work in, promoting health and hygiene to the IDPs and refugees that live here.
The order of sequence for the roll-out of these types of campaigns in general reflects established guidelines from EMERGENCY and/or other sources such as the World Health Organization (WHO).
 This campaign was carried out in Ashti camp, 30 minutes south of Sulaymaniyah. Our Medical Coordinator Vesna (seen here) from Serbia, who among other things, is responsible for attending health cluster meetings with our NGO partners, asked the nursing staff for statistical data generated from our clinic on worm presentations.
This campaign was carried out in Ashti camp, 30 minutes south of Sulaymaniyah. Our Medical Coordinator Vesna (seen here) from Serbia, who among other things, is responsible for attending health cluster meetings with our NGO partners, asked the nursing staff for statistical data generated from our clinic on worm presentations.
The first goal was to determine whether there was a need for this type of health campaign based on the number of visits we see for a given presentation. We soon realized that there was.
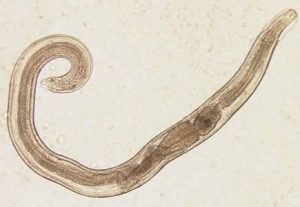 This is what we were up against. Meet Enterobius vermicularis, also known as the common pin worm. We had been receiving record number of visits to the clinic by children affected by this. And when infection in the camp is so widespread, individually treating symptomatic individuals as they present in clinic tends not to work as it may eradicate the infection in a few children, only then for them to go back home and reacquire it through siblings who had not yet had symptoms but were also infected. The treatment only kills active infection but does not prevent the reacquiring of it.
This is what we were up against. Meet Enterobius vermicularis, also known as the common pin worm. We had been receiving record number of visits to the clinic by children affected by this. And when infection in the camp is so widespread, individually treating symptomatic individuals as they present in clinic tends not to work as it may eradicate the infection in a few children, only then for them to go back home and reacquire it through siblings who had not yet had symptoms but were also infected. The treatment only kills active infection but does not prevent the reacquiring of it.
The only real, effective solution is to provide universal eradication treatment to those most infected.
Typically, this requires administration twice per year.
Though the most common symptoms are simply itching in the affected area, more serious symptoms include loss of appetite, weight loss, and stunted growth.
… Steady
Once a need has been established by our statistical record keeping, the Medical Coordinator and Chief Health Promoter then need to weigh up factors and determinants such as: man-hour requirement, clinic resources, availability of medication and overall budget.
 This is Anastasia from Ukraine, our International Health Promoter
This is Anastasia from Ukraine, our International Health Promoter
She is in charge of running the campaign. She has a team of about 8 local health promoters and an international nurse to help with execution of the campaign; the team broke up into 2-3 person pods, walked tent to tent and administered medication when possible. They would return later if the children weren’t home on the initial visit.
 Over nine days, we treated over 5,000 children between the age of 1-14, an estimated 99% of the camp’s child population.
Over nine days, we treated over 5,000 children between the age of 1-14, an estimated 99% of the camp’s child population.
In an effort to help ensure education, contribute to the internal camp economy, and ultimately engage the people of Iraq with medical independence, EMERGENCY promotes training and employment of camp members who are interested in becoming local Health Promoters.





