One hypothesis could be that the engine has started working again and the boat is sailing towards Sicily, but we have no evidence of this.

EMERGENCY presents the report ‘A QUIET REVOLUTION’ The EMERGENCY Anabah Maternity Centre and female empowerment.
2019 is the 41st year of war in Afghanistan. The country has been devastated by a never-ending conflict that has caused huge damage, left hundreds of thousands of casualties, and created an even higher number of internally displaced persons and refugees.
The war has seriously compromised the country’s infrastructure, including the national health service. Women in particular have difficulties in accessing treatment.
EMERGENCY has been working in Afghanistan since 1999. In 2003, we built a Maternity Centre in Anabah, the Panjshir Valley, that continues to be the only free, specialist structure in the area.

‘A Quiet Revolution’ is EMERGENCY’s report analysing the impact that a free, specialist Maternity Centre can have on the health and societal role of the women who are part of it: both patients and staff. The report also examines how the system can provide a model to be replicated in other parts of the country, as well as in other countries with few resources.
EMERGENCY’s Maternity Centre offers gynaecological, obstetric and neonatal care, as well as family planning and contraception services. It is also a recognised training centre for our local staff, all female. To date, hundreds of nurses and obstetricians have been trained at the facility, along with many doctors.

EMERGENCY’s research for the report began in autumn 2018, through surveys among 300 patients at the Maternity Centre, 50 health workers at the Centre and two First Aid Posts, and interviews with 20 other health workers.
The female motality rate in Afghanistan is over 50% higher than the male mortality rate. 1 in 14 women dies during pregnancy or childbirth. The infant mortality rate is also high, with 1 child in 18 dying before their 5th birthday (80% of these before their 1st).
Safety was reported as the primary obstacle to receiving medical assistance by 40% of the women interviewed, well ahead of distance from healthcare facilities, at 10%. Family and cultural attitudes also constitute a serious obstacle according to 31% of respondents.
“Childbirth is something almost all women go through in Afghanistan and EMERGENCY’s Maternity Centre is a microcosm reflecting the differences within the country. Many patients arrive from rural areas in the provinces of Panjshir and neighbouring Parwan and Kapisa. They are often illiterate and attracted primarily by the lack of cost and wide range of treatment. Many others come from the capital, Kabul, and are normally better educated and better placed to make independent decisions on their pregnancy, in the knowledge that the quality of medical assistance at EMERGENCY is very high. However, the interviews with mothers do reveal difficulties they have in common in accessing medical treatment, such as a lack of safety due to fighting, resistance from family members due to cultural and religious taboos, costs, and long distances. The research does not take into account those women who have not managed to get obstetrical treatment, but those who have explained that certain features of EMERGENCY’s Maternity Centre have made such treatment more accessible for women and more accepted by the population at large.”
– Fabrizio Foschini, Researcher at the Afghanistan Analysts Network
When EMERGENCY built its Maternity Centre in Anabah, it was unthinkable for most local families that their wives and daughters would work side-by-side with international staff. They feared that close contact with international staff would put the honour and reputation of young women working there at risk.
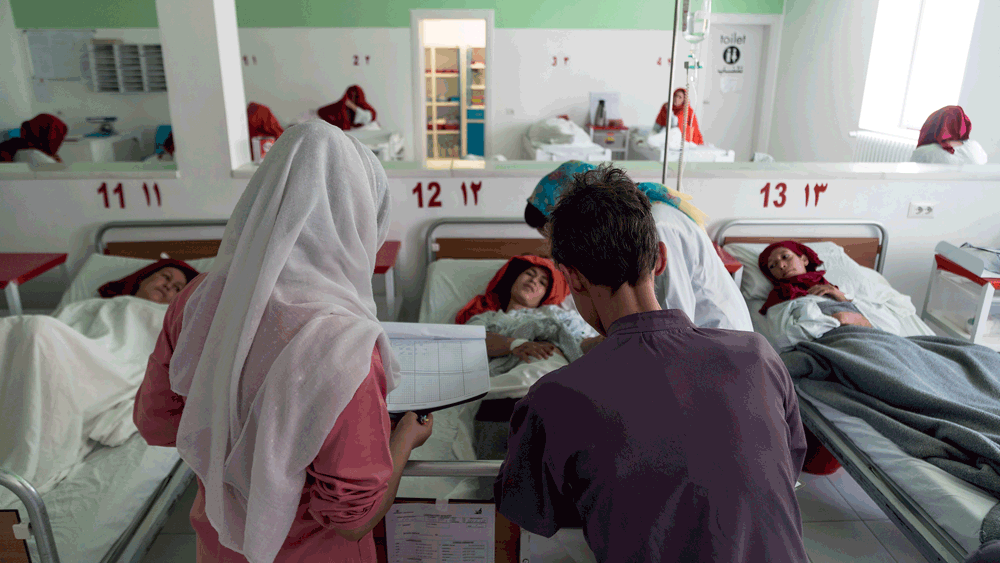
Although it took a long time for local people to accept them, today our international staff are generally considered by our patients as having a beneficial impact, greatly improving medical services. In spite of the early naysayers, EMERGENCY’s Maternity Centre is now able to deliver 600 babies a month, and 70% of the women interviewed have specifically chosen EMERGENCY for the quality of its treatment.
“In the last 12 years I have seen thousands of babies born, but more importantly I have seen women being reborn and growing – our obstetricians, nurses and young doctors. These are women who have studied, worked and fought, against a lot of prejudice, and sometimes even threats, to become professionals who are working with passion, intelligence and, above all, empathy. The Maternity Centre in Anabah is a little world, where women save each other’s lives.”
– Raffaela Baiocchi, EMERGENCY O&G Medical Division
Educated women who commit to a career seem to have a chance to change their role in Afghan society.
Decisions on women’s health pose an important question, because they are directly linked to women’s freedom to move outside their homes and other permitted places. Paradoxically, it is in this sphere that even EMERGENCY’s workers, with their medical skills, have to submit to their husbands’ authority.
Education seems to make a difference. Just 6.3% of illiterate women make decisions at home, compared with 21.1% of women who have been to school.

“Becoming active participants in society. That is the Afghan women’s delicate and silent revolution. Through our practical, day-to-day work, we are supporting them in that struggle. EMERGENCY’s reputation among local people has not only made our work at the Maternity Centre possible – it has helped shape a new role for female health workers in the region. Today, the women who work with us are no longer tolerated as exceptions to the rule. They are quickly becoming respected members of their communities, promoters of change, and an example of how to overcome traditional roles,” says Rossella Miccio, President of EMERGENCY.
The Maternity Centre has therefore become somewhere women can fulfil a role in society, as mothers or health workers; assume a more active role in decisions on health; and even challenge social taboos and family concerns, to study or embark on a career.
The example of the Anabah Maternity Centre also reinforces the UN’s idea, in its ‘Standards for improving quality of maternal and newborn care in health facilities’, published by the WHO in 2016, that strategies for reducing maternal and neonatal death should concentrate on the quality of medical assistance and not only on its availability. In the last few decades, there have been global efforts to create as many programmes of professional assistance as possible for childbirth in health facilities, but they have not had positive effects on health.
The WHO defines quality of care as “the extent to which health care services provided to individuals and patient populations improve desired health outcomes. In order to achieve this, health care must be safe, effective, timely, efficient, equitable and people-centred.” What makes the difference is infrastructure, human resources, knowledge, and skills in the face of challenges.
The results of our research underline and support the idea that quality in medical assistance is essential to increasing the number of births overseen by qualified people or in hospitals, as well as to reaching targets in the field of maternal health.



